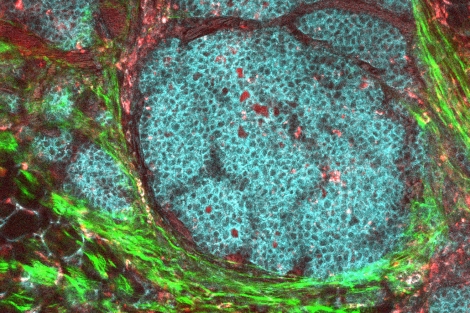
Riverside: A research team at the University of California, Riverside has
discovered a way for chemotherapy drug paclitaxel to target migrating,
or circulating, cancer cells, which are responsible for the development
of tumor metastases. Until now, paclitaxel has only been used to target rapidly dividing
cancer cells. The team was successful in getting the drug to piggyback
on 123B9, an agent they devised to target an oncogene
called EphA2 (ephrin type-A receptor 2). EphA2 spreads cancer by
allowing malignant cells to migrate from the primary tumor into
circulation and eventually to adhere to other tissues.
Only good, independent and reliable information about health from experts.
Showing posts with label chemotherapy. Show all posts
Showing posts with label chemotherapy. Show all posts
Thursday, May 10, 2018
Monday, May 7, 2018
Gene Mapping Lays Groundwork for Precision Chemotherapy
UCSF: Despite the great successes of targeted cancer drugs and the promise
of novel immunotherapies, the vast majority of people diagnosed with
cancer are still first treated with chemotherapy. Now a new study by
UCSF researchers using techniques drawn from computational biology could
make it much easier for physicians to use the genetic profile of a
patient’s tumor to pick the chemotherapy treatment with the fewest side
effects and best chance of success. “Since 95 percent of cancer patients still get chemo, we realized we
could make a major impact on cancer treatment by helping clinicians
prescribe the right chemotherapy drug,” said Sourav Bandyopadhyay, PhD, a professor of bioengineering and therapeutic sciences in UCSF’s Schools of Pharmacy and Medicine and senior author on the new study.
New test could tell doctors whether patients will respond to chemotherapy
Purdue: Less than half the patients diagnosed with cancer
respond favorably to chemotherapy, but a new method for testing how
patients will respond to various drugs could pave the way for more
personalized treatment. Using Doppler light scattering, like a weather
radar, researchers can determine how a patient will respond to
chemotherapy even before they begin treatment. “Doppler weather radar sends electromagnetic
waves into clouds, and while you don’t see individual rain droplets, you
pick up the overall motion of the raindrops. What you create with this
is a 3-D map of cloud motion,” said David Nolte, the Edward M. Purcell
Distinguished Professor of Physics and Astronomy at Purdue University.
“We’re looking at the motion inside living tissue rather than rain
droplets, and we’re using infrared light instead of radar. It’s like
watching the weather inside living tissue as the tissue is affected by
cancer drugs.”
Tuesday, February 28, 2017
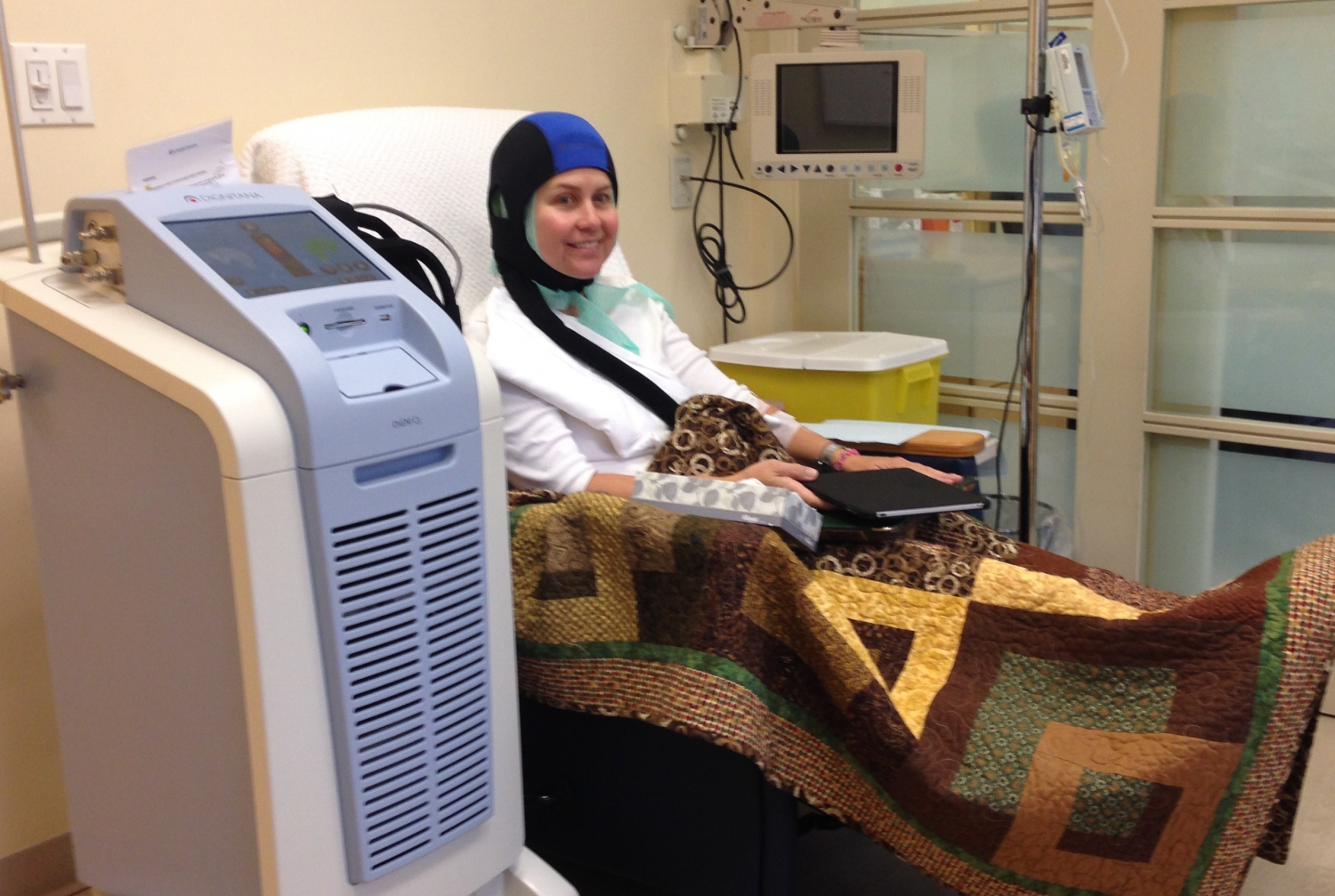
Scalp Cooling Can Help Some Breast Cancer Patients Retain Hair
Cornell: Scalp cooling can lessen some chemotherapy-induced hair loss – one of
the most devastating hallmarks of cancer – in certain breast cancer
patients, according to a new multicenter study from UC San Francisco,
Weill Cornell Medicine, NewYork-Presbyterian and three other medical
centers. A majority of the study’s patients, all women with
stage 1 or 2 breast cancer who underwent scalp cooling, retained more
than half of their hair after completing chemotherapy, the investigators
learned. The study, published which tracks patients over five years,
used standardized photographs to grade hair loss. The study was published Feb. 14 in JAMA, the Journal of the American Medical Association.
Thursday, February 16, 2017
Scientists create scorecard index for heart-damaging chemo drugs
Stanford: Researchers at the Stanford University School of Medicine
used heart muscle cells made from stem cells to rank commonly used
chemotherapy drugs based on their likelihood of causing lasting heart
damage in patients. Drugs known as tyrosine kinase inhibitors can be an effective
treatment for many types of cancers, but they also have severe and
sometimes fatal side effects. Using lab-grown heart cells,
Stanford researchers were able to assess the drugs’ various effects on
heart muscle cells, including whether the cells survived, were able to
beat rhythmically and effectively, responded appropriately to
electrophysiological signals and communicated with one another.
Saturday, November 12, 2016
Harmful effects of a commonly used cancer drug can be alleviated by using gene therapy
Helsinki: Doxorubicin treatment, which is commonly used in a variety of
cancers, leads to cardiac atrophy and body wasting. Researchers from the
Wihuri Research Institute and the University of Helsinki found that in
mouse heart, doxorubicin leads to blood vessel rarefaction, which was
prevented by treatment with gene therapy using the VEGF-B growth factor.
Wednesday, November 9, 2016
New discovery in understanding chemotherapy resistance could prevent cancer cells fighting back
 Sheffield: Scientists have made an important breakthrough in understanding why some cancer cells become resistant to chemotherapy. Researchers from the University of Sheffield have identified a
specific modification to proteins that wrap around the DNA of cancer
cells, protecting them from chemotherapy treatment. Most types of chemotherapy and radiotherapy kill cancer cells by
causing many breaks in the DNA – the blueprint that carries the
information needed to make proteins, and for cells to survive.
Sheffield: Scientists have made an important breakthrough in understanding why some cancer cells become resistant to chemotherapy. Researchers from the University of Sheffield have identified a
specific modification to proteins that wrap around the DNA of cancer
cells, protecting them from chemotherapy treatment. Most types of chemotherapy and radiotherapy kill cancer cells by
causing many breaks in the DNA – the blueprint that carries the
information needed to make proteins, and for cells to survive.Sunday, November 6, 2016
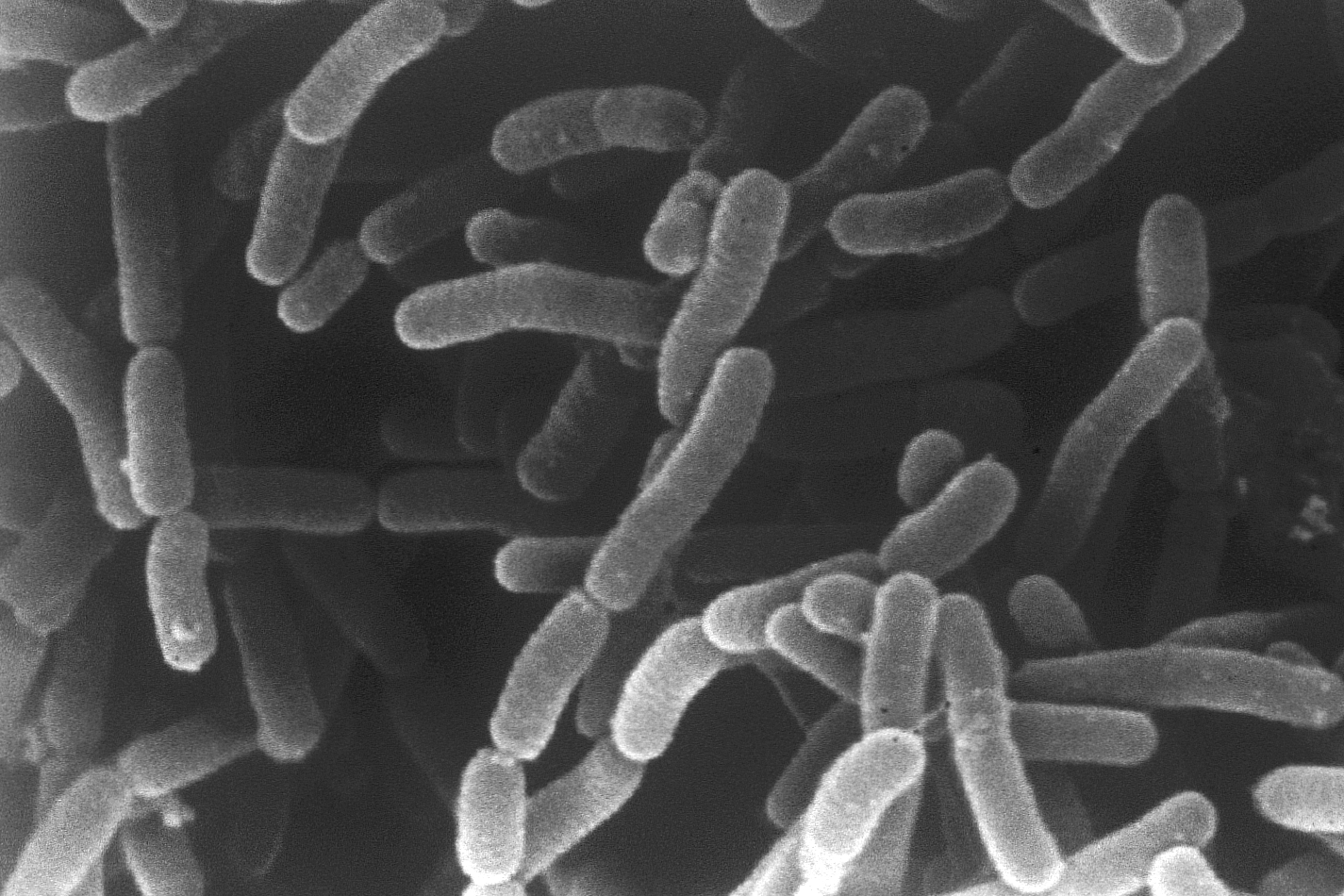
The gut microbiota to the rescue of chemotherapies
INSERM: Two species of bacteria present in the gut boost the efficacy of cyclophosphamide-based chemotherapies by optimising the antitumour immunity induced by this drug. This is reported by researchers from Inserm, Gustave Roussy, CNRS, Institut Pasteur Lille, and the Universities of Paris Sud and of Lille in an article published on 4 October in the journal Immunity.Recent studies have shown that certain gut microbes encourage tumours to grow, whereas others contribute to making cancer treatments more effective. It remained necessary to identify the nature and mode of action of the bacterial species capable of optimising the antitumour response induced by chemotherapy.
Sunday, May 24, 2015
Ginger for chemotherapy-induced nausea: Does it work?
Mayo Clinic: Can taking ginger for nausea reduce or eliminate nausea and vomiting caused by chemotherapy? There is evidence that when taken with standard anti-nausea
medications, ginger may be helpful in further reducing or eliminating
nausea and vomiting during and after chemotherapy treatments. Results from two studies of adults who took ginger for nausea showed
that various doses of ginger before starting chemotherapy treatments
helped to reduce the severity of nausea. In these studies, participants
began taking ginger orally three days prior to starting chemotherapy.
The ginger was taken in addition to a standard medication prescribed to
reduce nausea and vomiting. A small number of participants reported side
effects including heartburn, bruising, flushing and rash.
Wednesday, April 29, 2015
How to identify drugs that work best for each patient
MIT: Implantable device could allow doctors to test cancer drugs in patients before prescribing chemotherapy. More
than 100 drugs have been approved to treat cancer, but predicting which
ones will help a particular patient is an inexact science at best. A new device developed at MIT may change that. The implantable
device, about the size of the grain of rice, can carry small doses of up
to 30 different drugs. After implanting it in a tumor and letting the
drugs diffuse into the tissue, researchers can measure how effectively
each one kills the patient’s cancer cells. Such a device could eliminate much of the guesswork now involved in
choosing cancer treatments, says Oliver Jonas, a postdoc at MIT’s Koch
Institute for Integrative Cancer Research and lead author of a paper
describing the device in the April 22 online edition of Science Translational Medicine.
Friday, April 3, 2015
Fish oil could counteract chemo
Scimex: Dutch and Japanese scientists have found that people consuming herring
and mackerel fish, as well as three kinds of fish oils, actually raised
their blood levels of a certain chemo-counteracting fatty acid,
indicating that chemotherapy patients should avoid them during
treatment. Previous studies in mice have indicated that certain fatty
acids in fish oils may actually counteract the tumour-fighting effects
of chemotherapy, a finding which has implications for the growing use of
supplements by cancer patients during their treatments.
Thursday, April 2, 2015
Potential resistance to Chemotherapy after Consuming Fatty Acid in Fish, Fish Oil
JAMA: Researchers found that consuming the fish herring and mackerel, as
well as three kinds of fish oils, raised blood levels of the fatty acid
16:4(n-3), which experiments in mice suggest may induce resistance to
chemotherapy used to treat cancer, according to a study published online
by JAMA Oncology.
Thursday, March 26, 2015
Wednesday, March 25, 2015
Blood test could help bowel cancer patients avoid drug side-effects
 Manchester: Colorectal, or bowel, cancer is the second biggest cancer killer in
Europe. It is most commonly treated with a combination of chemotherapy
agents, and outcome can be improved by using additional drugs. However,
this multi-drug approach can increase side-effects such as hair loss,
low white blood cell count, diarrhoea and damage to the peripheral
nervous system. The team from Manchester counted tumour cells in a patient’s blood sample as a way of predicting who might benefit most.
Manchester: Colorectal, or bowel, cancer is the second biggest cancer killer in
Europe. It is most commonly treated with a combination of chemotherapy
agents, and outcome can be improved by using additional drugs. However,
this multi-drug approach can increase side-effects such as hair loss,
low white blood cell count, diarrhoea and damage to the peripheral
nervous system. The team from Manchester counted tumour cells in a patient’s blood sample as a way of predicting who might benefit most.Wednesday, March 4, 2015
New nanodevice defeats drug resistance
MIT: Tiny particles embedded in gel can turn off drug-resistance genes, then release cancer drugs. Chemotherapy
often shrinks tumors at first, but as cancer cells become resistant to
drug treatment, tumors can grow back. A new nanodevice developed by MIT
researchers can help overcome that by first blocking the gene that
confers drug resistance, then launching a new chemotherapy attack
against the disarmed tumors.
Thursday, January 22, 2015
Step closer to predicting cancer patients' drug toxicity
Adelaide University. Australia: Being able to predict that a patient will adversely react to a drug that's meant to be treating them is a key aim of personalised medicine, and could help to improve the patient's overall treatment. Researchers at the University of Adelaide are now one step closer to accurately predicting which cancer patients will experience severe toxicity from chemotherapy.
Tuesday, October 7, 2014
Gemzar
Gemcitabine is used to treat pancreatic
cancer, breast cancer, ovarian cancer, and lung cancer, and may be used
for other cancers as well.
Gemcitabine is a member of a group of chemotherapy drugs known as anti-metabolites. It prevents cells from making DNA, which stops cell growth and causes the cells to die.
Gemcitabine is a member of a group of chemotherapy drugs known as anti-metabolites. It prevents cells from making DNA, which stops cell growth and causes the cells to die.
Monday, October 6, 2014
Abseamed
-
Abseamed
is a solution for injection. It is available in pre-filled syringes
that contain between 1,000 and 40,000 international units (IU) of the active substance, epoetin alfa.
Abseamed is a ‘biosimilar medicine'. This means that Abseamed is similar to and contains the same active substance as a biological medicine that is already authorised in the European Union (EU), which is known as the ‘reference medicine’. The reference medicine for Abseamed is Eprex/Erypo.
Abseamed is used to treat anemia.
Labels
Abseamed,
anaemia,
anemia,
cancer,
chemotherapy,
EPO,
Eprex,
Erypo,
erythropoietin,
surgery
Subscribe to:
Comments (Atom)