University of Michigan :The new approach blocks the interaction between cancer cells and immune receptors, showing promise in mice.
A
team of researchers has found disrupting the interaction between cancer
cells and certain immune cells is more effective at killing cancer
cells than current immunotherapy treatments.
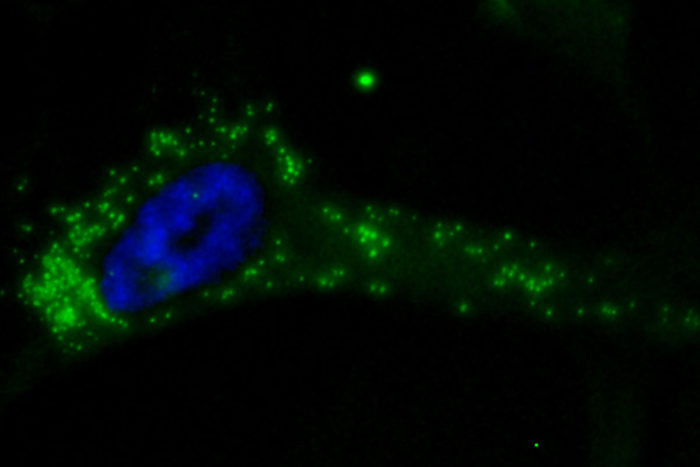
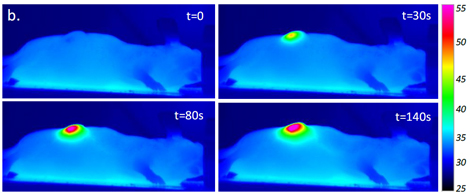
The findings, which include studies in cell lines and animal models, appeared in JCI Insight and focus on a protein called CD6 as a target for a new approach to immunotherapy.