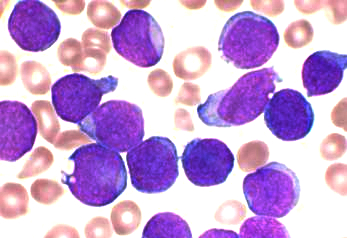
The researchers were able to demonstrate that a targeted drug-based inactivation of the two chromatin regulators will interrupt the self-renewing program, thereby causing leukemia cells to revert to normal blood cells. The results have been published in the October issue of Cancer Discovery.
Acute myeloid leukemia (AML) refers to a group of disorders that are also known as blood cancer. AML is an aggressive disease of malignant immature blood cells which, if left untreated, almost always causes the death of the affected patient. The established method of treatment is the use of a combination of various chemotherapeutic agents. However, dependent on the genetic subtype and the age of the patient, only about half of those with AML respond to this kind of treatment.
The goal of current research is thus to develop more efficient and less toxic forms of treatment. To achieve this, Dr. Michael Kühn of the University Medical Center of Johannes Gutenberg University Mainz (JGU) has been collaborating with the work groups of Professor Scott Armstrong in New York and Boston. They built on the relatively recent scientific discovery that changes to the "packaging structure" of DNA can contribute to the development of cancers. These chemical modifications particularly occur in the so-called histone proteins. These proteins are responsible for the coiling of DNA in mammalian cells. Various chemical modifications of these histone proteins will result in an increase or decrease in the relevant gene activity. DNA wrapped around histones is also called chromatin. Accordingly, the proteins writing, reading, or removing the chemical modifications of histones are called chromatin regulators.
These modifications represent a layer of information that can be passed from a parent cell to a daughter cell but is not encoded in the DNA sequence. This field of research is therefore known as "epigenetics". Medical research focusing on epigenetics is currently trying to block the enzymes that regulate these changes thereby silencing cancer promoting genes. One example of such research is the study undertaken by Dr. Michael Kühn and his colleagues. Its subject is the NPM1-mutated (NPM1mut) AML subtype, which is one of the most common leukemias in adults under the age of 60 years.
It has been known for quite some time that NPM1mut AMLs are associated with the activation of the so-called homeobox (HOX) stem cell genes. The HOX genes play a fundamental role in the developmental processes of organisms. They are particularly responsible for the self-renewal of blood stem cells. It has been assumed that activation of HOX genes turns normal blood cells into leukemia cells by initiating stem cell-like self-renewal. However, it has been unclear to date how this activation occurs. In an attempt to answer this question, the researchers undertook a targeted manipulation of leukemia cell DNA in the lab. Using a relatively new technology called CRISPR/Cas9, they managed to accurately cut out specific DNA sequences from leukemia cells. This enabled them to analyze the functioning of two proteins, namely, the mixed lineage leukemia (MLL) protein and the disruptor of telomeric silencing 1-like (DOT1L) protein.
Based on these experiments, the researchers were able to demonstrate that the survival of NPM1mut leukemia cells depends on these two proteins. Both proteins belong to a group of regulators that control chromatin and thus an important structural component of the cell nucleus. The researchers then used two highly specific chemical agents to block the specific functions of those proteins. While they were able to block DOT1L directly using an inhibitor substance currently being tested in a clinical trial for a different type of leukemia, a direct drug-based inhibition of MLL proved impossible. The researchers therefore inhibited chromatin binding of MLL using drugs that target this protein indirectly.
Both drugs reduced the activity of the homeobox stem cell genes in NPM1mut leukemia cells, while the combination of the two compounds resulted in nearly complete inactivation of these genes. Following combined exposure to the two substances, the leukemia cells underwent substantial changes and, to the surprise of the researchers, started to turn back into normal blood cells.
The described approach represents the first molecularly targeted treatment of NPM1mut leukemias by reversing a key mechanism of leukemogenesis and builds a basis for future clinical trials assessing these drugs in patients with NPM1mut leukemia.