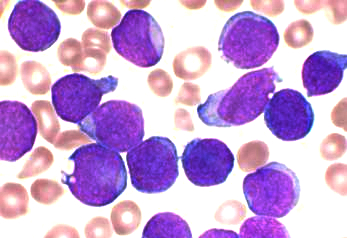
UCSF: A team led by UCSF researchers has discovered how a commonly
administered vaccine protects against acute lymphoblastic leukemia
(ALL), the most common type of childhood cancer. The Haemophilus influenzae Type b (Hib) vaccine not only
prevents ear infections and meningitis caused by the Hib bacterium, but
also protects against ALL, which accounts for approximately 25 percent
of cancer diagnoses among children younger than 15 years, according to
the National Cancer Society. The Hib vaccine is part of the standard
vaccination schedule recommended by the Centers for Disease Control and
is routinely given to children in four doses before 15 months of age.
Only good, independent and reliable information about health from experts.
Showing posts with label Acute Lymphoblastic Leukemia. Show all posts
Showing posts with label Acute Lymphoblastic Leukemia. Show all posts
Sunday, May 24, 2015
Tuesday, February 24, 2015
T-cell therapy clinical trial now offered to cancer patients at C.S. Mott Children’s Hospital
Michigan University. US: Innovative treatment uses patient’s own immune cells against acute lymphoblastic leukemia. A clinical trial using T-cell therapy that uses the
patients’ own immune cells to hunt down cancer cells is now being
offered at the University of Michigan’s C.S. Mott Children’s Hospital.
Tuesday, December 23, 2014
US. FDA approves Blincyto to treat a rare form of acute lymphoblastic leukemia
The U.S. Food and Drug Administration today approved Blincyto (blinatumomab) to treat patients with Philadelphia chromosome-negative precursor B-cell acute lymphoblastic leukemia (B-cell ALL), an uncommon form of ALL.
Precursor B-cell ALL is a rapidly growing type of cancer in which the bone marrow makes too many B-cell lymphoblasts, an immature type of white blood cell. The Philadelphia chromosome is an abnormality that sometimes occurs in the bone marrow cells of leukemia patients. The National Cancer Institute estimates that 6,020 Americans will be diagnosed with ALL and 1,440 will die from the disease in 2014.
Blincyto is an example of immunotherapy, a treatment that uses certain parts of a person’s immune system to fight diseases such as cancer. Blincyto is the first approved drug that engages the body’s T-cells, a type of white blood cell or lymphocyte, to destroy leukemia cells. The drug acts as a connector between a protein called CD19, which is found on the surface of most B-cell lymphoblasts, and CD3, a protein on T-cell lymphocytes. It is intended for patients whose cancer returned after treatment (relapsed) or did not respond to previous treatment (refractory).
“Immunotherapies, especially Blincyto with its unique mechanism of action, are particularly promising for patients with leukemia,” said Richard Pazdur, M.D., director of the Office of Hematology and Oncology Products in the FDA’s Center for Drug Evaluation and Research. “Recognizing the potential of this novel therapy, the FDA worked proactively with the sponsor under our breakthrough therapy designation program to facilitate the approval of this novel agent.”
The FDA granted Blincyto breakthrough therapy designation, priority review and orphan product designation because the sponsor demonstrated through preliminary clinical evidence that the drug may offer a substantial improvement over available therapies; the drug had the potential, at the time the application was submitted, to be a significant improvement in safety or effectiveness in the treatment of a serious condition; and the drug is intended to treat a rare disease, respectively. Blincyto is being approved more than five months ahead of the prescription drug user fee goal date of May 19, 2015, the date the agency was scheduled to complete review of the application.
The safety and effectiveness of Blincyto were evaluated in a clinical study involving 185 adults with Philadelphia chromosome-negative relapsed or refractory precursor B-cell ALL. All participants were treated with Blincyto for at least four weeks via infusion, a method used to inject treatment into the bloodstream using a needle. Results showed 32 percent of participants had no evidence of disease (complete remission) for approximately 6.7 months.
Blincyto is being approved under the FDA’s accelerated approval program, which allows approval of a drug to treat a serious or life-threatening disease based on clinical data showing the drug has an effect on a surrogate endpoint reasonably likely to predict clinical benefit to patients. This program provides earlier patient access to promising new drugs while the company conducts confirmatory clinical trials. The FDA is requiring Blincyto’s manufacturer to conduct a study to verify that the drug improves survival in participants with relapsed or refractory Philadelphia-negative precursor B-cell ALL.
Blincyto carries a boxed warning alerting patients and health care professionals that some clinical trial participants had problems with low blood pressure and difficulty breathing (cytokine release syndrome) at the start of the first treatment, experienced a short period of difficulty with thinking (encephalopathy) or other side effects in the nervous system. The most common side effects seen in Blincyto-treated participants were fever (pyrexia), headache, swelling of tissues (peripheral edema), fever with a low number of white blood cells (febrile neutropenia), nausea, low potassium (hypokalaemia), fatigue, constipation, diarrhea and tremor.
The FDA approved Blincyto with a Risk Evaluation and Mitigation Strategy (REMS), which consists of a communication plan to inform health care providers about the serious risks and the potential for preparation and administration errors.
Blincyto is marketed by Thousand Oaks, California-based Amgen Inc.
The FDA, an agency within the U.S. Department of Health and Human Services, promotes and protects the public health by, among other things, assuring the safety, effectiveness, and security of human and veterinary drugs, vaccines and other biological products for human use, and medical devices. The agency also is responsible for the safety and security of our nation’s food supply, cosmetics, dietary supplements, products that give off electronic radiation, and for regulating tobacco products.
More with FDA
Precursor B-cell ALL is a rapidly growing type of cancer in which the bone marrow makes too many B-cell lymphoblasts, an immature type of white blood cell. The Philadelphia chromosome is an abnormality that sometimes occurs in the bone marrow cells of leukemia patients. The National Cancer Institute estimates that 6,020 Americans will be diagnosed with ALL and 1,440 will die from the disease in 2014.
Blincyto is an example of immunotherapy, a treatment that uses certain parts of a person’s immune system to fight diseases such as cancer. Blincyto is the first approved drug that engages the body’s T-cells, a type of white blood cell or lymphocyte, to destroy leukemia cells. The drug acts as a connector between a protein called CD19, which is found on the surface of most B-cell lymphoblasts, and CD3, a protein on T-cell lymphocytes. It is intended for patients whose cancer returned after treatment (relapsed) or did not respond to previous treatment (refractory).
“Immunotherapies, especially Blincyto with its unique mechanism of action, are particularly promising for patients with leukemia,” said Richard Pazdur, M.D., director of the Office of Hematology and Oncology Products in the FDA’s Center for Drug Evaluation and Research. “Recognizing the potential of this novel therapy, the FDA worked proactively with the sponsor under our breakthrough therapy designation program to facilitate the approval of this novel agent.”
The FDA granted Blincyto breakthrough therapy designation, priority review and orphan product designation because the sponsor demonstrated through preliminary clinical evidence that the drug may offer a substantial improvement over available therapies; the drug had the potential, at the time the application was submitted, to be a significant improvement in safety or effectiveness in the treatment of a serious condition; and the drug is intended to treat a rare disease, respectively. Blincyto is being approved more than five months ahead of the prescription drug user fee goal date of May 19, 2015, the date the agency was scheduled to complete review of the application.
The safety and effectiveness of Blincyto were evaluated in a clinical study involving 185 adults with Philadelphia chromosome-negative relapsed or refractory precursor B-cell ALL. All participants were treated with Blincyto for at least four weeks via infusion, a method used to inject treatment into the bloodstream using a needle. Results showed 32 percent of participants had no evidence of disease (complete remission) for approximately 6.7 months.
Blincyto is being approved under the FDA’s accelerated approval program, which allows approval of a drug to treat a serious or life-threatening disease based on clinical data showing the drug has an effect on a surrogate endpoint reasonably likely to predict clinical benefit to patients. This program provides earlier patient access to promising new drugs while the company conducts confirmatory clinical trials. The FDA is requiring Blincyto’s manufacturer to conduct a study to verify that the drug improves survival in participants with relapsed or refractory Philadelphia-negative precursor B-cell ALL.
Blincyto carries a boxed warning alerting patients and health care professionals that some clinical trial participants had problems with low blood pressure and difficulty breathing (cytokine release syndrome) at the start of the first treatment, experienced a short period of difficulty with thinking (encephalopathy) or other side effects in the nervous system. The most common side effects seen in Blincyto-treated participants were fever (pyrexia), headache, swelling of tissues (peripheral edema), fever with a low number of white blood cells (febrile neutropenia), nausea, low potassium (hypokalaemia), fatigue, constipation, diarrhea and tremor.
The FDA approved Blincyto with a Risk Evaluation and Mitigation Strategy (REMS), which consists of a communication plan to inform health care providers about the serious risks and the potential for preparation and administration errors.
Blincyto is marketed by Thousand Oaks, California-based Amgen Inc.
The FDA, an agency within the U.S. Department of Health and Human Services, promotes and protects the public health by, among other things, assuring the safety, effectiveness, and security of human and veterinary drugs, vaccines and other biological products for human use, and medical devices. The agency also is responsible for the safety and security of our nation’s food supply, cosmetics, dietary supplements, products that give off electronic radiation, and for regulating tobacco products.
More with FDA
Tuesday, August 26, 2014
Acute Lymphocytic Leukemia
Also called: ALL, Acute lymphoblastic leukemia
Leukemia is cancer of the white blood cells. White blood cells help your body fight infection. Your blood cells form in your bone marrow. In leukemia, however, the bone marrow produces abnormal white blood cells. These cells crowd out the healthy blood cells, making it hard for blood to do its work. In acute lymphocytic leukemia (ALL), also called acute lymphoblastic leukemia, there are too many of specific types of white blood cells called lymphocytes or lymphoblasts. ALL is the most common type of cancer in children.
Possible risk factors for ALL include being male, being white, previous chemotherapy treatment, exposure to radiation, and for adults, being older than 70.
Symptoms of ALL include:
More about acute lymphoblastic leukemia
Leukemia is cancer of the white blood cells. White blood cells help your body fight infection. Your blood cells form in your bone marrow. In leukemia, however, the bone marrow produces abnormal white blood cells. These cells crowd out the healthy blood cells, making it hard for blood to do its work. In acute lymphocytic leukemia (ALL), also called acute lymphoblastic leukemia, there are too many of specific types of white blood cells called lymphocytes or lymphoblasts. ALL is the most common type of cancer in children.
Possible risk factors for ALL include being male, being white, previous chemotherapy treatment, exposure to radiation, and for adults, being older than 70.
Symptoms of ALL include:
- Weakness or feeling tired
- Fever
- Easy bruising or bleeding
- Bleeding under the skin
- Shortness of breath
- Weight loss or loss of appetite
- Pain in the bones or stomach
- Pain or a feeling of fullness below the ribs
- Painless lumps in the neck, underarm, stomach, or groin
More about acute lymphoblastic leukemia
Friday, May 11, 2012
Acute Lymphoblastic Leukemia
Introduction
Every year about 10,000 children develop cancer in the US. Acute lymphoblastic leukemia (ALL), a rapidly progressing blood cancer, accounts for a quarter of these childhood cancers. Normally, cells in the bone marrow (the spongy material inside bones) develop into lymphocytes (white blood cells that fight infections), red blood cells (which carry oxygen round the body), platelets (which prevent excessive bleeding), and granulocytes (another type of white blood cell). However, in ALL, genetic changes in immature lymphocytes (lymphoblasts) mean that these cells divide uncontrollably and fail to mature.
Every year about 10,000 children develop cancer in the US. Acute lymphoblastic leukemia (ALL), a rapidly progressing blood cancer, accounts for a quarter of these childhood cancers. Normally, cells in the bone marrow (the spongy material inside bones) develop into lymphocytes (white blood cells that fight infections), red blood cells (which carry oxygen round the body), platelets (which prevent excessive bleeding), and granulocytes (another type of white blood cell). However, in ALL, genetic changes in immature lymphocytes (lymphoblasts) mean that these cells divide uncontrollably and fail to mature.
Subscribe to:
Posts (Atom)