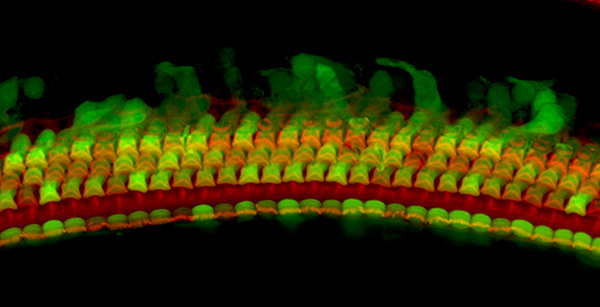
While previous vectors have only been able to penetrate the cochlea’s inner hair cells, one of the papers shows that a new synthetic vector, Anc80, safely transfers genes to the hard-to-reach outer hair cells when introduced into the cochlea.
This study’s three senior investigators were Jeffrey Holt, HMS professor of otolaryngology and of neurology at Boston Children’s; Konstantina Stankovic, HMS associate professor of otolaryngology and otologic head and neck surgeon at Mass. Eye and Ear; and Luk Vandenberghe, HMS assistant professor of ophthalmology at Mass. Eye and Ear who led the development of Anc80 in 2015.
“Now you can whisper, and they can hear you.” —Gwenaëlle Géléoc“We have shown that Anc80 works remarkably well in terms of infecting cells of interest in the inner ear,” said Stankovic. “With more than 100 genes already known to cause deafness in humans, there are many patients who may eventually benefit from this technology.”
The second study, led by Gwenaëlle Géléoc, HMS assistant professor of otolaryngology and a member of the F.M. Kirby Neurobiology Center at Boston Children’s, used Anc80 to deliver a specific corrected gene in a mouse model of Usher syndrome, the most common genetic form of deaf-blindness that also impairs balance function.
“This strategy is the most effective one we’ve tested,” said Géléoc. “Outer hair cells amplify sound, allowing inner hair cells to send a stronger signal to the brain. We now have a system that works well and rescues auditory and vestibular function to a level that’s never been achieved before.”
Ushering in gene therapy for deafness
Géléoc and colleagues at Boston Children’s studied mice with a mutation in Ush1c, the same mutation that causes Usher type 1C in humans. The mutation causes a protein called harmonin to be nonfunctional. As a result, the sensory hair cell bundles that receive sound and signal the brain deteriorate and become disorganized, leading to profound hearing loss.
When a corrected Ush1c gene was introduced into the inner ears of the mice, the inner and outer hair cells in the cochlea began to produce normal full-length harmonin. The hair cells formed normal bundles that responded to sound waves and signaled the brain, as measured by electrical recordings.
Most important, deaf mice treated soon after birth began to hear.
Géléoc and colleagues showed this first in a startle box, which detects whether a mouse jumps in response to sudden loud sounds. When they next measured responses in the auditory regions of the brain, a more sensitive test, the mice responded to much quieter sounds: 19 of 25 mice heard sounds quieter than 80 decibels, and a few heard sounds as soft as 25-30 decibels, like normal mice.
“Now you can whisper, and they can hear you,” said Géléoc.
Improving communication
Margaret Kenna, HMS professor of otolaryngology and a specialist in genetic hearing loss at Boston Children’s who does research on Usher syndrome, is excited about the work.
“Anything that could stabilize or improve native hearing at an early age would give a huge boost to a child’s ability to learn and use spoken language,” she said.
“Cochlear implants are great, but your own hearing is better in terms of range of frequencies; nuance for hearing voices, music and background noise; and figuring out which direction a sound is coming from. In addition, the improvement in balance could translate to better and safer mobility for Usher syndrome patients.”
Restoring balance
Since patients—and mice—with Usher 1C also have balance problems caused by hair-cell damage in the vestibular organs, the researchers also tested whether gene therapy restored balance.
It did, eliminating the erratic movements of mice with vestibular dysfunction and, in another test, enabling the mice to stay on a rotating rod for longer periods without falling off.
Further work is needed before the technology can be brought to patients.
One caveat is that the mice were treated right after birth; hearing and balance were not restored when gene therapy was delayed 10 to 12 days. The researchers will do further studies to determine the reasons for this. However, when treated early, the effects persisted for at least six months, with only a slight decline between 6 weeks and 3 months.
The researchers also hope to test gene therapy in larger animals and plan to develop novel therapies for other forms of genetic hearing loss.
Combining hearing and blindness therapies
“I believe our studies take an important step toward unlocking a future of hearing gene therapy.” —Luk VandenbergheUsher syndrome also causes blindness by causing the light-sensing cells in the retina to gradually deteriorate. Although these studies did not test for vision restoration, gene therapy in the eye has already begun for other disorders.
“We already know the vector works in the retina,” said Géléoc, “and because deterioration is slower in the retina, there is a longer window for treatment.”
“Progress in gene therapy for blindness is much further along than for hearing, and I believe our studies take an important step toward unlocking a future of hearing gene therapy,” said Vandenberghe. “In the case of Usher syndrome, combining both approaches to ultimately treat both the blinding and hearing aspects of disease is very compelling, and something we hope to work toward.”
“This is a landmark study,” said Holt, director of otolaryngology research at Boston Children’s who was also a co-author on the second paper. “Here we show, for the first time, that by delivering the correct gene sequence to a large number of sensory cells in the ear, we can restore both hearing and balance to near-normal levels.”
The work was supported by the Bertarelli Foundation, Kidz-b-Kidz Foundation, Foundation Fighting Blindness, Jeff and Kimberly Barber Gene Therapy Research Fund, and Manton Center for Orphan Disease Research at Boston Children’s Hospital.
Vandenberghe is an inventor on Anc80 (patent #WO/2015/054653) and other gene transfer technologies for which he receives royalties. These technologies are licensed to several gene therapy companies, some of which fund research in Vandenberghe’s laboratory (Selecta Biosciences and Lonza Houston).
Adapted from a joint news release from Boston Children’s and Mass. Eye and Ear.