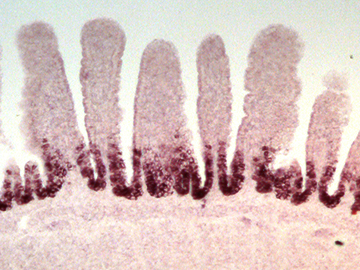
Harvard: Mommy, where do intestinal stem cells come from? All right, it’s not likely a kindergartner would ask such a question. But evolutionary biologists want to know. Adult intestinal stem cells live at the bases of our villi, the tiny,
fingerlike protuberances that line the intestines and absorb nutrients. There, the stem cells constantly churn out new intestinal cells to replace those being destroyed by corrosive digestive juices.
The researchers asked: How and when do these stem cells appear in the right place so they can do their job?
Studying mice and chicks, whose intestinal formation is similar to
ours, the team found that the entire intestinal lining has stem cell
properties at first. As the embryo develops, all but a few cells lose
this potential.
“This lends support to the theory that adult stem cells are remnants of a more general pool of cells in the embryo,” said Amy Shyer,
who conducted the work as a graduate student in the lab of Cliff Tabin
at Harvard Medical School and is now a Miller Fellow at the University
of California, Berkeley.
As for why these cells are restricted to the villi bases, or crypts,
the researchers believe the structure of the developing intestine
determines which cells receive signals from neighboring tissues that
say, “Stop being stem cells.”
About two weeks into development, the intestine, initially a smooth
tube, starts to form mountainous zigzags that will ultimately become
villi. Cells at the peaks are exposed to signals that suppress stem cell
properties, while cells in the valleys don’t receive them.
“This opens a new door conceptually,” said Shyer. “Tissues that start
out uniform but then need to set up regions with regular patterns—which
happens in the gut, skin, lungs and other organs during embryonic
development—might coopt these natural changes in architecture to dictate
signals that specify cell fate locally.”
“It’s likely that this powerful mechanism is used in many other parts of the embryo in addition to the developing gut,” said Tabin,
the George Jacob and Jacqueline Hazel Leder Professor of Genetics and
head of the Department of Genetics at HMS, who was senior author of the
paper.
The team’s findings were published online in Cell.
“While enormous progress has been made in determining how stem cells
act and how they’re maintained, much less attention has been paid to how
pools of stem cells are apportioned to the correct location in the body
as an embryo develops,” Tabin added.
“This study provides some of the first insights into this problem, in
the context of the extremely well-studied intestinal stem cells, which
are critical for renewal of the gut and also a key target in GI tract
cancers.”
The team doesn’t expect the results to translate to the clinic
anytime soon. Shyer, Tabin and their colleagues are mainly driven by a
desire to understand more about how our bodies, and the bodies of other
organisms, form and function.
However, it’s possible that what they found will one day be applied
to engineering tissue or to fighting cancers that occur when intestinal
stem cells go into overdrive.
“There are very fundamental aspects of our tissues we don’t
understand. In the context of potentially engineering some of these
things in a lab, or better repairing them when there’s some sort of
mistake in the program, I really think studies like this will help us
get a better handle on how tissue construction takes place,” said Shyer,
who was first author of the study.
“It’s a relief when you find places like this where things are
self-organizing,” said Shyer. “If we want to build a gut and put stem
cells in place, we don’t have to instruct every stem cell where to go.
Nature has built that into the program.”
This research was supported by a grant from the National Institutes of Health (R01 HD047360) and by the MacArthur Foundation.