RNSA: Too little sleep takes a toll on your heart, according to a new study to
be presented today at the annual meeting of the Radiological Society of
North America (RSNA). People who work in fire and emergency medical services, medical
residencies and other high-stress jobs are often called upon to work
24-hour shifts with little opportunity for sleep. While it is known that
extreme fatigue can affect many physical, cognitive and emotional
processes, this is the first study to examine how working a 24-hour
shift specifically affects cardiac function.
"For the first time, we have shown that short-term sleep deprivation
in the context of 24-hour shifts can lead to a significant increase in
cardiac contractility, blood pressure and heart rate," said study author
Daniel Kuetting, M.D., from the Department of Diagnostic and
Interventional Radiology at the University of Bonn in Bonn, Germany.
For the study, Dr. Kuetting and colleagues recruited 20 healthy
radiologists, including 19 men and one woman, with a mean age of 31.6
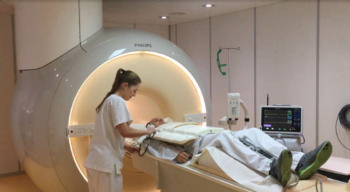
years. Each of the study participants underwent cardiovascular magnetic
resonance (CMR) imaging with strain analysis before and after a 24-hour
shift with an average of three hours of sleep.
"Cardiac function in the context of sleep deprivation has not
previously been investigated with CMR strain analysis, the most
sensitive parameter of cardiac contractility," Dr. Kuetting said.
The researchers also collected blood and urine samples from the participants and measured blood pressure and heart rate.
Following short-term sleep deprivation, the participants showed
significant increases in mean peak systolic strain (pre = -21.9; post =
-23.4), systolic (112.8; 118.5) and diastolic (62.9; 69.2) blood
pressure and heart rate (63.0; 68.9). In addition, the participants had
significant increases in levels of thyroid stimulating hormone (TSH),
thyroid hormones FT3 and FT4, and cortisol, a hormone released by the
body in response to stress.
Although the researchers were able to perform follow-up examinations
on half of the participants after regular sleep, Dr. Kuetting notes that
further study in a larger cohort is needed to determine possible
long-term effects of sleep loss.
"The study was designed to investigate real-life work-related sleep
deprivation," Dr. Kuetting said. "While the participants were not
permitted to consume caffeine or food and beverages containing
theobromine, such as chocolate, nuts or tea, we did not take into
account factors like individual stress level or environmental stimuli."
As people continue to work longer hours or work at more than one job
to make ends meet, it is critical to investigate the detrimental effects
of too much work and not enough sleep. Dr. Kuetting believes the
results of this pilot study are transferable to other professions in
which long periods of uninterrupted labor are common.
"These findings may help us better understand how workload and shift duration affect public health," he said.
Co-authors on the study are Andreas Feisst, M.D., Rami Homsi, M.D.,
Julian A. Luetkens, M.D., Daniel Thomas, M.D., Ph.D., Hans H. Schild,
M.D., and Darius Dabir, M.D.