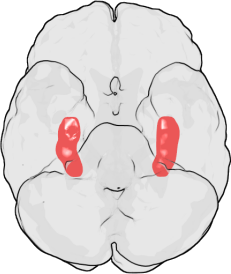
Sydney: The brains of people with recurrent depression have a significantly
smaller hippocampus - the part of the brain most associated with forming
new memories - than healthy individuals, a new global study of nearly
9,000 people reveals. Published in Molecular Psychiatry, the
ENIGMA study is co-authored by University of Sydney scholars at the
Brain and Mind Research Institute. The research is the largest
international study to compare brain volumes in people with and without
major depression. It highlights the need to identify and treat
depression effectively when it first occurs, particularly among
teenagers and young adults. Using magnetic resonance imaged (MRI)
brain scans, and clinical data from 1,728 people with major depression
and 7,199 healthy individuals, the study combined 15 datasets from
Europe, the USA and Australia.
Major depression is a common
condition affecting at least one in six people during their lifetime. It
is a serious clinical mood disorder in which feelings of sadness,
frustration, loss, or anger interfere with a person's everyday life for
weeks, months or years at a time.
Key findings
The key
finding that people with major depression have a smaller hippocampus
confirms earlier clinical work conducted at the BMRI. In this study, the
key finding was largely explained by subjects with recurrent
depression. People with recurrent depression represented 65 per cent of
study subjects with major depression.
People with an early age of
onset of major depression (before the age of 21 years) also had a
smaller hippocampus than healthy individuals, consistent with the notion
that many of these young people go on to have recurrent disorders.
However,
people who had a first episode of major depression (34 per cent of
study subjects with major depression) did not have a small hippocampus
than healthy individuals, indicating that the changes are due to the
adverse effects of depressive illness on the brain.
Commentary
"These
findings shed new light on brain structures and possible mechanisms
responsible for depression," says Associate Professor Jim Lagopoulos of
the University of Sydney's Brain and Mind Research Institute.
"Despite
intensive research aimed at identifying brain structures linked to
depression in recent decades, our understanding of what causes
depression is still rudimentary.
"One reason for this has been the
lack of sufficiently large studies, variability in the disease and
treatments provided, and the complex interactions between clinical
characteristics and brain structure."
Commenting on the clinical
significance of the findings, Co-Director of the Brain and Mind Research
Institute, Professor Ian Hickie says: "This large study confirms the
need to treat first episodes of depression effectively, particularly in
teenagers and young adults, to prevent the brain changes that accompany
recurrent depression.
"This is another reason that we need to
ensure that young people receive effective treatments for depression - a
key goal of our Centre of Research Excellence in
Optimising Early
Interventions for Young People with Emerging Mood Disorder. "This new
finding of smaller hippocampal volume in people with major depression
may offer some support to the neurotrophic hypothesis of depression,"
adds Jim Lagopoulos.
"This hypothesis argues that a range of
neurobiological processes such as elevated glucocorticoid levels in
those with chronic depression may induce brain shrinkage.
"Clearly,
there's a need for longitudinal studies that can track changes in
hippocampal volume among people with depression over time, to better
clarify whether hippocampal abnormalities result from prolonged duration
of chronic stress, or represent a vulnerability factor for depression,
or both," he said.